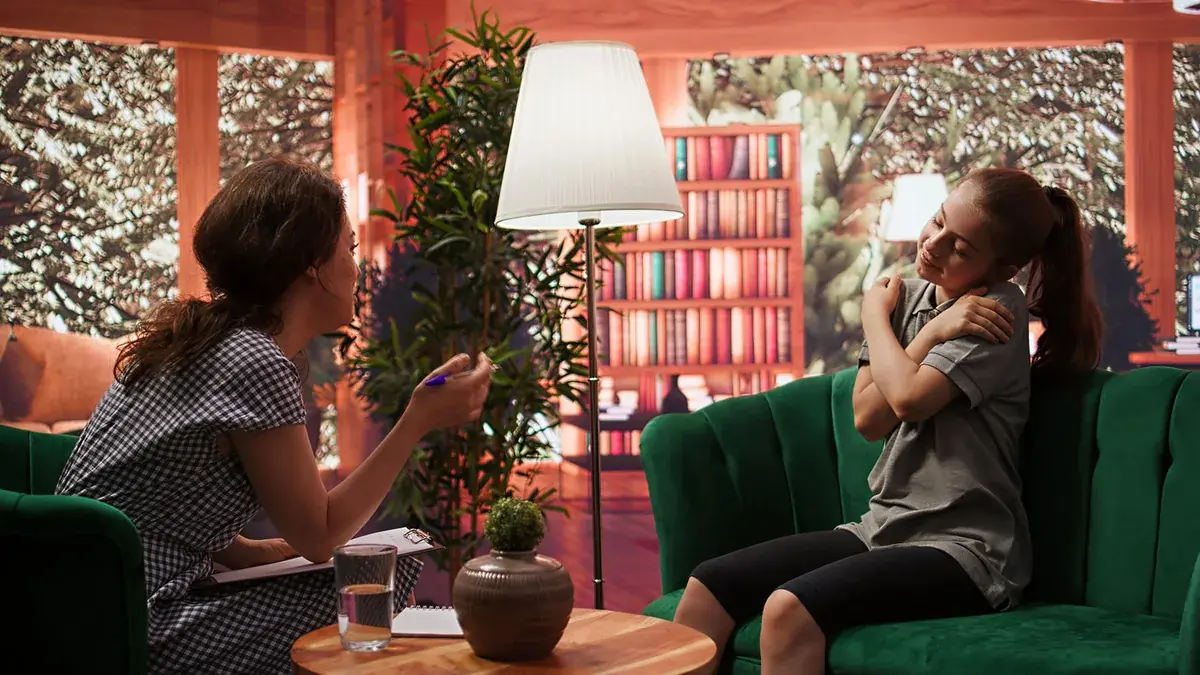Substance Use Disorder Therapy: Evidence-Based Behavioral Treatments for Recovery
Medication addresses the neurochemistry of addiction; therapy teaches the skills and strategies needed to sustain long-term recovery. At KwikPsych, we emphasize evidence-based behavioral therapies that have demonstrated effectiveness in helping people build lasting sobriety.
While Dr. Monika Thangada provides psychiatric evaluation and medication management, we work collaboratively with licensed therapists specializing in addiction counseling and behavioral treatment.
Why Behavioral Therapy Is Essential
Substance use disorder involves learned behaviors reinforced over time:
- Environmental cues: Sights, sounds, places trigger automatic cravings
- Emotional patterns: Stress, boredom, anger, loneliness become cues for use
- Thinking patterns: "I can't handle this without a drink" or "I deserve to get high"
- Social patterns: Relationships, social situations built around substance use
- Identity: Self-perception as "an addict"
Medication reduces physical cravings and withdrawal discomfort, but behavioral therapy:
- Rewires automatic responses to triggers
- Teaches coping skills for managing cravings and difficult emotions
- Identifies and changes thought patterns that drive use
- Rebuilds relationships and social connections
- Reestablishes meaning and purpose beyond substance use
- Prevents relapse by preparing for high-risk situations
Cognitive-Behavioral Therapy (CBT) for Addiction
CBT is one of the most extensively researched and effective treatments for substance use disorder. It's based on the principle that our thoughts, feelings, and behaviors are interconnected, and changing one aspect changes the others.
How CBT Works
The addiction cycle:
- Trigger: Environmental cue (place, person, emotion, stress) or internal cue (craving, boredom)
- Thought: Automatic thought in response to trigger ("I've had a rough day; I deserve to get high")
- Emotion: Emotional response (relief at the thought, anticipation)
- Craving: Intense desire to use
- Behavior: Use of the substance
Breaking the cycle:
- Identify triggers early
- Recognize automatic thoughts
- Challenge and change thoughts
- Develop alternative emotional responses
- Choose alternative behaviors
Core CBT Components for Addiction
1. Trigger Identification and Management
Common triggers:
- Environmental: Specific places (bar, dealer's house), objects (paraphernalia), people (using friends)
- Emotional: Stress, anxiety, depression, anger, loneliness, boredom
- Physical: Fatigue, pain, hunger, withdrawal symptoms
- Social: Peer pressure, arguments, social rejection
- Temporal: Anniversaries, holidays, specific times of day
Trigger identification exercise:
- Track when cravings occur and what preceded them
- Recognize patterns (what consistently triggers use)
- Rate intensity of triggers
- Identify which are most problematic
Trigger management strategies:
- Avoidance: Eliminate or minimize exposure to high-risk triggers (if possible)
- Exposure and coping: Gradually expose to triggers while practicing coping skills (if avoidance isn't possible)
- Environmental change: Change living situation, friend group, daily routine to reduce triggers
- Stimulus control: Removing cues and paraphernalia
2. Coping Skills Development
Coping strategies for managing cravings and triggers:
Cognitive coping:
- Recognizing automatic thoughts ("I can't handle this without using")
- Challenging thoughts with evidence
- Replacing with realistic, adaptive thoughts ("I've managed hard things before; I can do this")
- Mindfulness: Observing cravings without acting on them
- Urge surfing: Recognizing that cravings come in waves and will pass
Behavioral coping:
- Distraction: Activities that divert attention (exercise, hobbies, calling a friend)
- Physical activity: Exercise reduces cravings and improves mood
- Breathing techniques: Deep breathing, box breathing to calm autonomic nervous system
- Relaxation: Progressive muscle relaxation, meditation
- Social support: Calling a sponsor, support group member, therapist, or trusted friend
- Pleasant activities: Engaging in activities that provide natural reward (time with family, hobbies, entertainment)
Interpersonal coping:
- Assertiveness: Saying no to offers of substances
- Conflict resolution: Managing disagreements without escalation
- Communication: Expressing needs clearly
- Seeking help: Knowing when and how to reach out
3. Thinking Pattern Work (Cognitive Restructuring)
People with substance use disorders often have thinking patterns that support continued use:
Common problematic thoughts:
- "I can't handle stress without a substance"
- "I've already used once today; I might as well continue"
- "I deserve to use after my hard work"
- "One use won't hurt; I can control it"
- "I'm no good; I've failed too many times"
Cognitive restructuring process:
- Identify the automatic thought
- Examine evidence: What's true? What's not true about this thought?
- Generate alternatives: What's a more balanced, realistic thought?
- Evaluate alternatives: Which thoughts are more helpful and true?
- Practice: Rehearse new thoughts so they become automatic
Example:
- Original thought: "I can't handle this stress without getting high"
- Examining evidence: "I have handled stress before. I have a job, I managed my responsibilities. I have coping skills I've learned."
- Alternative: "This is stressful, and I can handle it. I'll exercise, call my therapist, and take it one step at a time."
4. Problem-Solving and Life Skills
Many people with substance use disorders have avoided developing healthy coping and problem-solving skills. CBT teaches:
- Problem definition: Clearly identifying what the actual problem is
- Generating solutions: Brainstorming multiple options without judgment
- Evaluating options: Pros and cons of each solution
- Implementing: Choosing and executing a solution
- Evaluating outcomes: Assessing whether the solution worked
Common life skill areas:
- Time management and planning
- Financial management
- Job seeking and workplace skills
- Conflict resolution
- Communication skills
- Self-care (sleep, nutrition, hygiene, exercise)
5. Relapse Prevention Planning
(Detailed below)
Duration and Format of CBT
- Typical duration: 16-20 weekly sessions (3-5 months) for initial phase, then less frequent maintenance
- Session length: 50-60 minutes
- Individual vs. group: Both formats available; often combination works well
- Homework: Assignments between sessions to practice skills (tracking triggers, coping practice, thought records)
Effectiveness of CBT
Strong evidence shows CBT:
- Reduces substance use significantly
- Improves coping skills and confidence in managing triggers
- Decreases craving intensity
- Works well combined with medication-assisted treatment
- Maintains benefits over time
Motivational Interviewing (MI)
Many people with substance use disorder are ambivalent about change. They recognize problems from use but also experience benefits (mood enhancement, escape from pain, social connection). Motivational interviewing works with this ambivalence rather than against it.
Core Principles of MI
1. Partnership: Therapist and client work together, not in a confrontational dynamic
2. Evoking: The therapist brings out the client's own reasons for change, rather than imposing reasons
3. Collaboration: Decisions about treatment are collaborative; client autonomy is respected
4. Autonomy: Recognizing that ultimate change comes from the individual's motivation and choice
MI Techniques
1. Open-Ended Questions
Rather than yes/no questions, open-ended questions elicit fuller responses:
- Instead of: "Have you thought about quitting?" (Yes/No)
- Ask: "What do you think might happen if you continued using?" or "What would be different in your life if you weren't using?"
This allows clients to articulate their own concerns and motivations.
2. Reflective Listening
The therapist demonstrates understanding by reflecting back what they heard:
- Client: "I know my drinking is out of control, but I don't know how to have fun anymore without it"
- Therapist reflection: "So you're recognizing the problem with drinking, and at the same time, you're worried that stopping would take away something important—the fun and relaxation. That's a real tension."
Reflections:
- Demonstrate genuine listening
- Allow clients to hear themselves
- Often prompt deeper reflection or change language
3. Developing Discrepancy
Gently helping the person recognize the gap between their values/goals and their current behavior:
- "You mentioned that being a good parent is really important to you. How do you think your substance use affects your ability to be the parent you want to be?"
- "You said you want to have your own place. How is your substance use helping or getting in the way of that goal?"
4. Rolling with Resistance
When someone expresses resistance to change ("I don't think treatment works," "I'm not an addict"), MI approaches this as information, not confrontation:
- Instead of: "You're in denial. You clearly have a problem"
- Respond: "You're not sure treatment would work for you. What would treatment need to look like for you to consider it?"
Rolling with resistance:
- Prevents defensive arguing
- Reduces polarization
- Often leads to deeper exploration
5. Supporting Self-Efficacy
Expressing confidence in the person's ability to change:
- "You've accomplished hard things before. What do you think gave you strength then?"
- "You recognized the problem, you reached out for help—those are steps that show you can take control"
Change Talk
In MI, therapists listen for "change talk"—language suggesting motivation to change:
- Desire: "I want to stop"; "I'd like to be different"
- Ability: "I could do this"; "I'm capable of handling it"
- Reasons: Specific benefits of changing ("My family would be proud")
- Taking steps: Actions already taken toward change
When clients say change talk, the therapist reinforces and amplifies it.
Timing of MI
- Most effective early in treatment when ambivalence is greatest
- Often used before and alongside other therapies
- Particularly helpful with mandated/legal system-involved clients who may initially be resistant
Effectiveness of MI
Evidence shows MI:
- Increases engagement in treatment
- Increases motivation to change
- Improves treatment outcomes
- Reduces defensive arguing and resistance
Contingency Management (Motivational Incentives)
Contingency management uses positive reinforcement to motivate behavior change. It's based on the principle that behaviors followed by positive consequences are more likely to be repeated.
How It Works
Rather than punishment for use, contingency management provides concrete rewards for:
- Submitting negative drug screens (abstinence)
- Attending therapy appointments
- Complying with medication
- Meeting specific treatment goals
Reward Systems
Voucher-based: Patients earn vouchers for target behaviors, exchangeable for goods or services
- Example: Negative drug screen = $10 voucher toward goods ($100 maximum per month)
Prize-based: Random reinforcement drawing; achieving target behavior enters you in drawing for prizes
- Example: Negative drug screen = entry into weekly drawing; 50% chance of winning a prize ($1-25)
Escalating schedules: Reinforcement value increases for continued successes
- Example: First month of abstinence = $10; second month = $15; third month = $20
Target Behaviors
- Negative urine drug screens
- Medication adherence
- Therapy attendance
- Engagement in support groups
- Achievement of personal goals (employment, family contact, etc.)
Effectiveness
Strong evidence shows contingency management:
- Reduces substance use during active reinforcement
- Effective across different substances of abuse
- Works well combined with other therapies
- Particularly good for initiating behavior change
Limitations:
- Effects may diminish when external reinforcement ends
- Requires sustained motivation after rewards stop
- Works best as part of comprehensive treatment including other therapies
12-Step Facilitation and Peer Support Programs
For many people, peer support and community are critical components of recovery. Several established peer support programs exist:
Alcoholics Anonymous (AA) and Narcotics Anonymous (NA)
Philosophy:
- Addiction is a disease, not a moral failing
- Acceptance of powerlessness over the substance
- Belief in a "higher power" (broadly interpreted)
- Recovery through 12 steps and group support
Structure:
- Free, peer-led meetings (open, closed, speaker, discussion formats)
- Typically 60-90 minutes
- Meetings throughout the day and week
- Sponsorship: one-on-one mentoring by someone stable in recovery
The 12 Steps (overview):
- Admit powerlessness over addiction
- Believe in a power greater than oneself
- Surrender to higher power
- Moral inventory
- Confession of wrongs
6-7. Character defects and removal
8-9. Amends to people harmed
10-12. Continued practice, spiritual growth, and helping others
Effectiveness:
- Peer support is powerful; community and belonging aid recovery
- Large population uses AA/NA effectively
- Meta-analyses show benefit comparable to other treatments
- Works well combined with professional treatment
SMART Recovery
Philosophy:
- Self-empowerment approach
- Cognitive-behavioral principles
- Focus on changing thoughts and behaviors
- Secular (no higher power requirement)
Tools:
- 4-Point Program: Building motivation, coping with urges, managing thoughts and behaviors, building a satisfying life
- Emphasizes personal responsibility and rational thinking
Structure: Free peer-led meetings; no sponsorship model but peer support
Best for: People who value cognitive-behavioral approach or secular approach; those uncomfortable with spiritual aspects of AA/NA
Refuge Recovery
Philosophy:
- Mindfulness-based approach
- Buddhist-inspired but secular
- Emphasis on present-moment awareness and compassion
Elements: Meditation, mutual support, sharing
Best for: People interested in mindfulness and meditation approaches; secular alternative with contemplative focus
Secular Organizations for Sobriety (SOS)
Philosophy:
- Secular approach; emphasizes personal responsibility
- Focus on rational self-empowerment
- Non-religious alternative to 12-step
Structure: Free peer meetings; emphasizes honesty and personal priority on sobriety
Multiple Pathways to Recovery
Not all people resonate with the same approach. Some people:
- Attend AA/NA
- Prefer SMART Recovery
- Use meditation-based programs
- Combine peer support with professional therapy only
The key is finding community, building relationships with others in recovery, and developing accountability.
12-Step Facilitation in Professional Treatment
Even therapists not part of AA/NA may use 12-step facilitation, introducing clients to meetings and supporting participation while maintaining professional boundaries.
Relapse Prevention
Relapse prevention is a structured approach to identifying high-risk situations and developing coping strategies before relapse occurs.
High-Risk Situations
Intrapersonal (within person) triggers:
- Negative emotional states: depression, anxiety, anger, boredom
- Positive emotional states (paradoxically): celebrations, success
- Physical states: pain, hunger, tiredness, illness
- Cravings and withdrawal symptoms
Interpersonal (social) triggers:
- Social pressure from friends/family
- Interpersonal conflict
- Desire to socialize ("everyone else is drinking")
- Relationship loss or rejection
Environmental triggers:
- Being in places associated with use
- Seeing cues (paraphernalia, money, people)
- Transition times or times of low structure
Relapse Prevention Plan Development
Step 1: Identify high-risk situations
- Client and therapist identify situations most likely to lead to relapse
- Rate probability and difficulty
- Prioritize top 5-10 situations
Step 2: Develop coping strategies
For each high-risk situation, create a detailed plan:
- What will you do immediately when you encounter this situation?
- Who will you call?
- Where will you go?
- What activities will you engage in?
- What thoughts will you practice?
Example:
- High-risk situation: Friday night after work; friends call inviting you to a bar
- Coping plan:
- Recognize this is a high-risk situation
- Remember my reasons for not drinking (health, family, job)
- Tell friends you can't go
- Go to the gym or attend a support group meeting instead
- Call my sponsor if I feel tempted
- Treat myself to something I enjoy (meal out, movie)
Step 3: Distinguish lapse from relapse
- Lapse: Single use or brief return to substance use
- Relapse: Full return to the pattern of use
Critical point: A lapse is not failure; it's information that treatment needs adjustment. Immediate response is key.
Response to lapse:
- Tell your therapist immediately
- Analyze what led to it
- Strengthen coping strategies in that area
- Increase support (more therapy, support groups)
- Adjust medication if needed
- Return to abstinence immediately
Mindset: Approaching a lapse as a learning opportunity rather than proof of failure makes returning to recovery much more likely.
Step 4: Build a recovery lifestyle
Beyond just avoiding use, relapse prevention includes building a positive life:
- Regular exercise and physical health
- Meaningful work or activities
- Relationships and social connection
- Hobbies and interests
- Spirituality or meaning-making
- Rest and leisure
- Sense of purpose
When life is fulfilling, the pull toward substance use diminishes.
Group Therapy for Substance Use Disorder
Group therapy offers unique benefits:
Advantages:
- Universality: "I'm not the only one going through this"
- Hope: Seeing others further along in recovery
- Peer support: Sharing experiences, advice, encouragement
- Social learning: Learning from others' experiences and strategies
- Community: Belonging and connection
- Cost: Often less expensive than individual therapy
- Interpersonal practice: Practicing communication and relationship skills
Typical format:
- 6-12 participants
- 60-90 minutes
- Once or twice weekly
- Open or closed (whether new members join ongoing groups)
- Led by therapist(s)
Topics in group:
- Sharing recovery stories
- Identifying triggers and coping strategies
- Supporting group members
- Building relationships without substance use
- Celebrating milestones
Family Therapy and Psychoeducation
Substance use disorder affects the whole family. Family therapy addresses:
Impact of Substance Use on Family
Consequences:
- Financial stress (money spent on substances)
- Emotional toll (worry, disappointment, anger)
- Broken trust
- Neglect of responsibilities (parenting, household)
- Conflict and arguments
- Violence in some cases
- Children's psychological effects
Family Therapy Goals
Education:
- Understanding addiction as a disease
- Recognizing co-dependence (family members' enabling behaviors)
- Understanding recovery process
Changing family dynamics:
- Establishing healthy boundaries
- Reducing enabling
- Improving communication
- Addressing family conflicts
- Rebuilding trust
Supporting recovery:
- Family members' role in supporting (without rescuing)
- Managing fear about relapse
- Rebuilding relationships
- Celebrating recovery milestones
Family Support Groups
Al-Anon (for families of alcoholics) and Nar-Anon (for families of people with opioid/drug addiction) offer:
- Support from others with similar experiences
- Education about addiction and recovery
- Tools for setting boundaries and self-care
- Acceptance that you can't control another's addiction
How to Access Therapy and Counseling
Through KwikPsych
Dr. Monika Thangada provides psychiatric evaluation and medication management. We refer to qualified therapists and counselors for behavioral therapy. Coordination of care ensures your psychiatrist and therapist are communicating.
Finding a Therapist
Qualities to look for:
- Licensed therapist (LCSW, LPC, LMFT, psychologist)
- Specialization in addiction/substance use
- Experience with your specific substance
- Experience with any co-occurring conditions (depression, anxiety, PTSD)
- Understanding of medication-assisted treatment
- Evidence-based approach (CBT, MI, contingency management)
Resources for finding therapists:
- Ask your psychiatrist for referrals
- SAMHSA Find Treatment Locator (samhsa.gov)
- Insurance provider's therapist directory
- Psychology Today therapist finder
- Local addiction treatment agencies
Levels of Therapy Services
- Individual counseling: One-on-one with therapist
- Group therapy: Structured group with multiple participants
- Intensive outpatient (IOP): Multiple group and individual sessions per week
- Peer support meetings: AA, NA, SMART Recovery, etc. (free)
What to Expect in Therapy
First session:
- Intake assessment: history, goals, previous treatment
- Psychoeducation about the therapy approach
- Agreement on treatment goals and frequency
- Homework assignment
Ongoing sessions:
- Review of previous week, challenges, victories
- Discussion of triggers and coping
- Skills practice and role-play
- Assignment of homework to practice between sessions
- Regular assessment of progress
Active participation:
- Therapies work best with genuine engagement
- Completing homework between sessions is important
- Honest discussion of challenges and relapses
- Willingness to practice new skills
Contact and Next Steps
To begin substance use disorder treatment with psychiatric medication management and therapy:
KwikPsych Psychiatry
Dr. Monika Thangada, MD
Phone: 737-367-1230
Address: 12335 Hymeadow Dr, Ste 450, Austin, TX 78750
Telehealth: Available across Texas
We'll conduct a comprehensive evaluation and connect you with experienced therapists specializing in substance use disorders.
Crisis Resources:
- Suicide & Crisis Lifeline: 988
- SAMHSA National Helpline: 1-800-662-4357 (free, confidential, 24/7)
- Emergency: 911
Disclaimer: This content is for education. Treatment should be individualized and provided by qualified professionals. If you're in crisis, please contact emergency services or the Suicide & Crisis Lifeline.
Insurance & Pricing
We accept most major insurance plans, including:
- Aetna
- Blue Cross Blue Shield (BCBS)
- Cigna
- UnitedHealthcare
- Superior HealthPlan / Ambetter
- Baylor Scott & White
- Oscar
- Optum
- Medicare
Plus others. See full list of accepted insurance plans →
Self-pay: Call us at 737-367-1230 to find out latest rates.